The Gut-Brain Connection: An Overview

The gut-brain axis forms a bustling superhighway of communication between your digestive tract and your brain, and new research is revealing just how vital this connection is. In 2024, a report in *Nature Reviews Neuroscience* highlighted that your gut is home to around 100 trillion microorganisms, which send signals to your brain through the vagus nerve and via chemical messengers. About 90% of the body’s serotonin—a neurotransmitter that stabilizes mood—is actually produced in the gut, not the brain. These gut microbes can also influence dopamine and gamma-aminobutyric acid (GABA) levels, which are both essential for mood regulation and cognitive function. The gut-brain axis has become a core focus for neuroscientists, as disruptions here are now strongly associated with anxiety, depression, and even cognitive decline. Researchers are especially interested in how gut health interventions may help prevent or treat mood disorders. In 2025, scientists are taking this connection more seriously than ever, with several clinical trials underway to test how improving gut health might relieve symptoms of depression and anxiety.
The Role of Gut Microbiome Diversity

A healthy gut relies on diversity—having a wide range of different bacterial species. The *Journal of Psychiatric Research* published findings in early 2025 showing that adults with greater gut microbiome diversity reported significantly fewer symptoms of anxiety and depression compared to those with less diverse microbiota. This diversity enables the gut to process a broader array of nutrients, resist pathogens, and maintain balance during stress. People who consume a varied diet rich in fiber, fermented foods, and prebiotics like onions and garlic often have higher gut diversity. The same study noted that individuals who ate at least 25 different plant-based foods weekly had a 32% lower risk of depressive symptoms than those who ate fewer than 10. These findings have led mental health professionals to recommend dietary variety as a concrete step for improving emotional resilience. Microbiome diversity is now seen as a marker not just for digestive health, but also for mental health.
The Impact of Diet on Gut Health

What you eat every day can radically influence your gut—and your mood. In 2024, the *American Journal of Clinical Nutrition* published a large-scale survey of 8,000 adults, finding that those who followed a Mediterranean diet, rich in fruits, vegetables, legumes, nuts, and olive oil, experienced a 28% lower rate of depression. Conversely, diets high in processed foods, artificial sweeteners, and refined sugars were strongly linked to imbalanced gut bacteria and higher rates of mood disorders. Omega-3 fatty acids, found in fatty fish and flaxseeds, are particularly beneficial for both the brain and the gut. B vitamins from leafy greens and whole grains also play a key role in neurotransmitter synthesis. The study concluded that intentional dietary choices can help restore healthy gut flora, improve neurotransmitter balance, and ultimately boost mental health.
The Role of Inflammation in Mood Disorders
Chronic inflammation is a silent saboteur when it comes to mental well-being. *Psychological Medicine* (2025) reported that individuals with major depressive disorder often have elevated levels of inflammatory markers, such as C-reactive protein (CRP). The gut microbiome strongly influences inflammation: specific beneficial bacteria produce short-chain fatty acids (SCFAs) like butyrate, which help dampen inflammatory responses throughout the body. If the gut barrier becomes “leaky” due to poor diet or stress, harmful bacteria and toxins can enter the bloodstream, triggering systemic inflammation that can reach the brain. This inflammatory cascade is now recognized as a contributor to anxiety, depression, and brain fog. New therapies are being explored to rebalance gut bacteria as a means of reducing brain inflammation and improving mood stability.
The Influence of Stress on Gut Health

Stress doesn’t just affect your mind; it can quickly disrupt your gut, too. A 2024 study in *Frontiers in Psychology* tracked over 1,200 adults and found that those experiencing chronic stress had a 40% reduction in beneficial gut bacteria like Lactobacillus and Bifidobacterium. Stress hormones such as cortisol alter the gut environment, leading to dysbiosis—a harmful imbalance of gut microbes. This, in turn, can increase gut permeability and inflammation, worsening anxiety and depressive symptoms. Techniques like mindfulness meditation, deep breathing, and yoga were found to help restore gut balance by lowering stress-induced inflammation. The bidirectional nature of the gut-brain axis means that reducing stress can directly support gut health, and vice versa.
Probiotics and Mental Health: What the Research Says

Probiotics, or “friendly” bacteria, have become a focus in the fight against mood disorders. A 2025 systematic review in *Nutrients* analyzed data from 33 clinical trials and found that supplementation with probiotic strains like Lactobacillus rhamnosus and Bifidobacterium longum led to a 25% reduction in self-reported anxiety and depressive symptoms. The studies noted that probiotics help restore balance in the microbiome, reduce inflammation, and even increase the production of neurotransmitters linked to positive moods. However, not all probiotics offer the same benefits, and individual responses vary depending on baseline gut health. Some experts advise combining probiotics with dietary changes for the greatest effect. New research is also exploring “psychobiotics”—probiotic strains specifically designed to target mood and cognition.
The Link Between Gut Health and Neurotransmitter Production
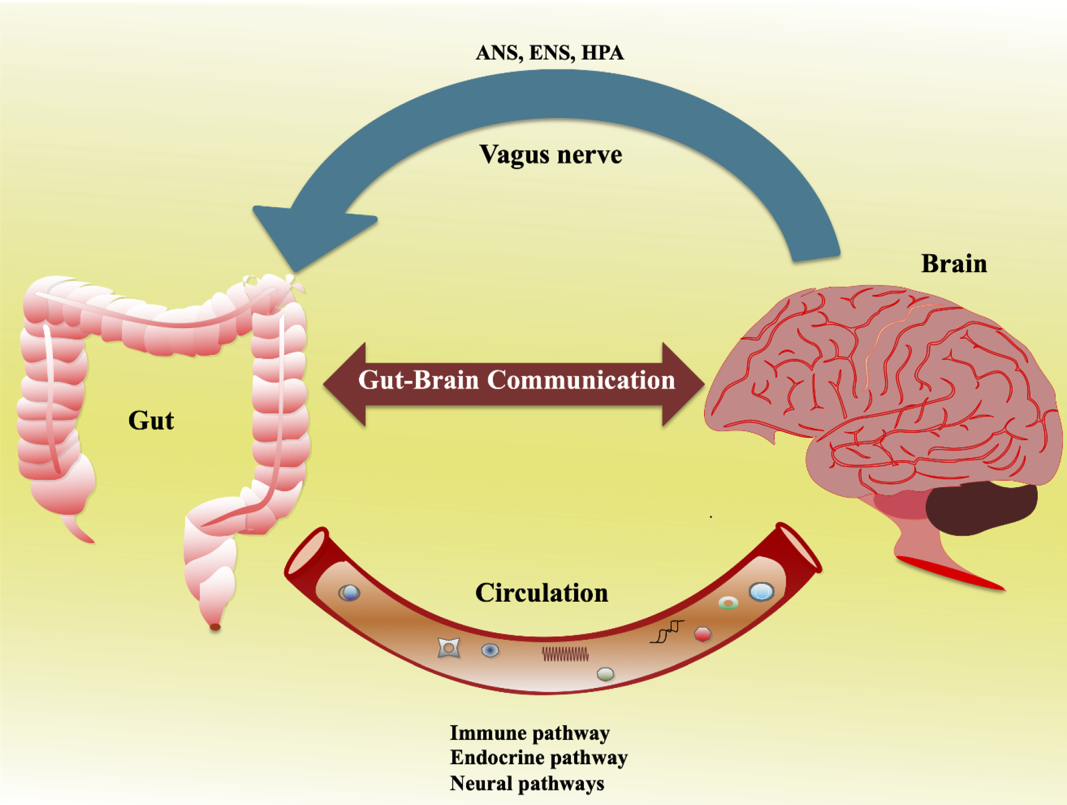
Gut bacteria are surprisingly powerful when it comes to producing and regulating neurotransmitters. The *Nature Communications* study from 2024 revealed that certain strains of gut bacteria can synthesize GABA, which helps calm the nervous system and reduce anxiety. Other microbes are involved in the production of dopamine and serotonin, both vital for feelings of well-being and motivation. The gut also influences levels of brain-derived neurotrophic factor (BDNF), which supports learning, memory, and neuroplasticity. Disruptions in these gut-driven processes can lead to mood swings, irritability, and even cognitive decline. Researchers are now focusing on how targeted changes to the gut microbiome could offer new hope for treating mood disorders.
Case Studies: Real-World Applications of Gut Health Interventions

Recent case studies bring the research to life with compelling results. In 2025, *Clinical Psychology Review* published a six-month intervention involving adults diagnosed with moderate depression. Participants followed a gut-friendly diet emphasizing fiber, fermented foods, and daily probiotic supplements. By the end of the study, 68% reported a significant reduction in depressive symptoms, and many noted improved sleep and energy. In another community-based program, individuals received hands-on nutrition education and support in meal planning. Over half reported notable improvements in mood, with fewer days lost to anxiety or low motivation. These real-world applications are fueling interest in gut-health-focused approaches as part of a holistic mental health strategy.
Future Directions in Gut Health Research

The pace of discovery in gut-brain research is accelerating. Emerging technologies like metagenomics and metabolomics, which allow scientists to analyze the gut microbiome in unprecedented detail, are uncovering new microbial species and metabolites linked to mental health. Personalized nutrition—creating diets tailored to an individual’s unique microbiome profile—is a hot topic for 2025, with several pilot programs underway in Europe and North America. Pharmaceutical companies are also developing psychobiotics—targeted probiotics designed to support brain health. As these innovations progress, experts predict gut health will become a standard part of mental health care protocols within the next decade.
Practical Tips for Improving Gut Health and Mood

Simple lifestyle changes can make a real difference for both gut and brain health. Experts recommend eating a wide variety of plant-based foods, aiming for at least 30 different types each week to maximize microbial diversity. Fermented foods like kefir, kimchi, and sauerkraut add beneficial bacteria directly to your gut. Regular exercise, even brisk walking, has been shown to boost the growth of healthy gut microbes and lower stress. Prioritizing 7–8 hours of quality sleep each night, staying well-hydrated, and limiting alcohol and highly processed foods are all practical steps. Social connection and mindful activities further support a balanced gut-brain axis, creating a foundation for improved mood and cognitive function.




