You wake up, check your blood sugar, and the number staring back at you makes no sense. You didn’t eat anything overnight. You were asleep. So why is it high? If this sounds familiar, you’re dealing with something millions of diabetics experience every single morning – and most don’t even know it has a name.
The dawn phenomenon is one of those frustrating quirks of diabetes that seems almost unfair. Your body does it automatically, quietly, while you’re completely unconscious. The good news? What you do in the hours before you fall asleep matters enormously. The right evening routine can be the difference between a frustrating morning number and one that starts your day on solid ground.
Here’s what the science actually says – and what you can do about it starting tonight. Let’s dive in.
Ritual 1: Skip the Late-Night Carbs (Seriously, This One Matters)

Let’s be real – late-night snacking feels harmless. A few crackers, a small bowl of cereal, maybe some fruit. But for someone with diabetes, this kind of high-carbohydrate eating before bed can directly worsen what you wake up to. The dawn phenomenon is not caused by a specific food or activity, but heavy dinners or snacks before bedtime may worsen it. That’s a crucial distinction, because it means the food choices you make at 9 or 10 p.m. are still having a conversation with your blood sugar by 5 a.m.
There is evidence that the timing and macronutrient content of meals in the evening can influence next-day glucose levels. In practical terms, this means swapping those bedtime carbs for something that digests more slowly. Eating a healthy snack before bedtime can help keep your sugar steady during the night – it is good to have some carbs and protein in your snack to slow down the process of how your body uses sugar. Think a small handful of almonds, some cheese, or Greek yogurt rather than toast or cookies.
Better control of morning glucose levels has been demonstrated by increasing the protein-to-carbohydrate ratio of the evening meal. The logic here is simple: protein digests more slowly than refined carbs, creating a far gentler overnight glucose curve. Think of it like choosing a long, slow-burning log for the fire rather than a handful of dry paper. The heat stays more even through the night.
Ritual 2: Take a Walk After Dinner

This one surprises people. Exercise? Before bed? Hear me out – there’s real science behind the after-dinner stroll, and it has nothing to do with burning calories in the traditional sense. Exercise can also help manage morning highs. If you have waning insulin, an after-dinner walk or other workout can help keep blood glucose down overnight. It doesn’t have to be intense. Even a gentle 20-minute walk can make a measurable difference.
Other studies have suggested that evening exercise may improve glycemia and reduce the dawn phenomenon. Exercising prior to overnight fasting may help improve hepatic insulin sensitivity, resulting in an attenuation of the early morning rise in endogenous glucose production responsible for the dawn phenomenon. That “early morning rise in endogenous glucose production” is essentially your liver releasing glucose in the pre-dawn hours – a key driver of the spike you see on your meter.
Here’s the catch, though. Timing matters. Use caution when exercising before bedtime. The blood glucose-lowering effects of exercise can last for hours, so if you work out before bed, you risk going low overnight. A walk right after dinner is the sweet spot – active enough to improve insulin sensitivity, but far enough from sleep that it won’t cause an overnight drop. Light and consistent beats intense and erratic every time.
Ritual 3: Go to Bed at the Same Time Every Night

This one feels almost too simple to be true. Honestly, I’d have dismissed it a few years ago too. But the connection between sleep consistency and blood sugar control is now well-supported by research. Lifestyle modification such as sleep hygiene plays a crucial role in glycemic control. Your body’s glucose metabolism is deeply tied to its internal clock, and when that clock gets scrambled, your blood sugar pays the price.
The dawn phenomenon is thought to be a consequence of an altered central circadian clock in the brain resulting in excessive hepatic glucose production during sleep and increased insulin resistance in the morning. In plain terms: your internal clock controls a big part of what your liver does while you’re asleep. Irregular sleep timing is like jamming a wrench into those gears. There is a bidirectional relationship between sleep disorders and diabetes: while diabetes and its complications lead to sleep disorders, disturbance in both sleep quality and quantity can lead to poorer diabetes control and a higher complication rate.
Poor sleep quality is associated with lower time in range and greater glycemic variability, so improving sleep quality could improve glycemic control. Going to bed and waking up at consistent times each day is one of the most underrated, zero-cost interventions available to anyone managing blood sugar. It’s not glamorous, but it works.
Ritual 4: Check and Log Your Bedtime Blood Sugar
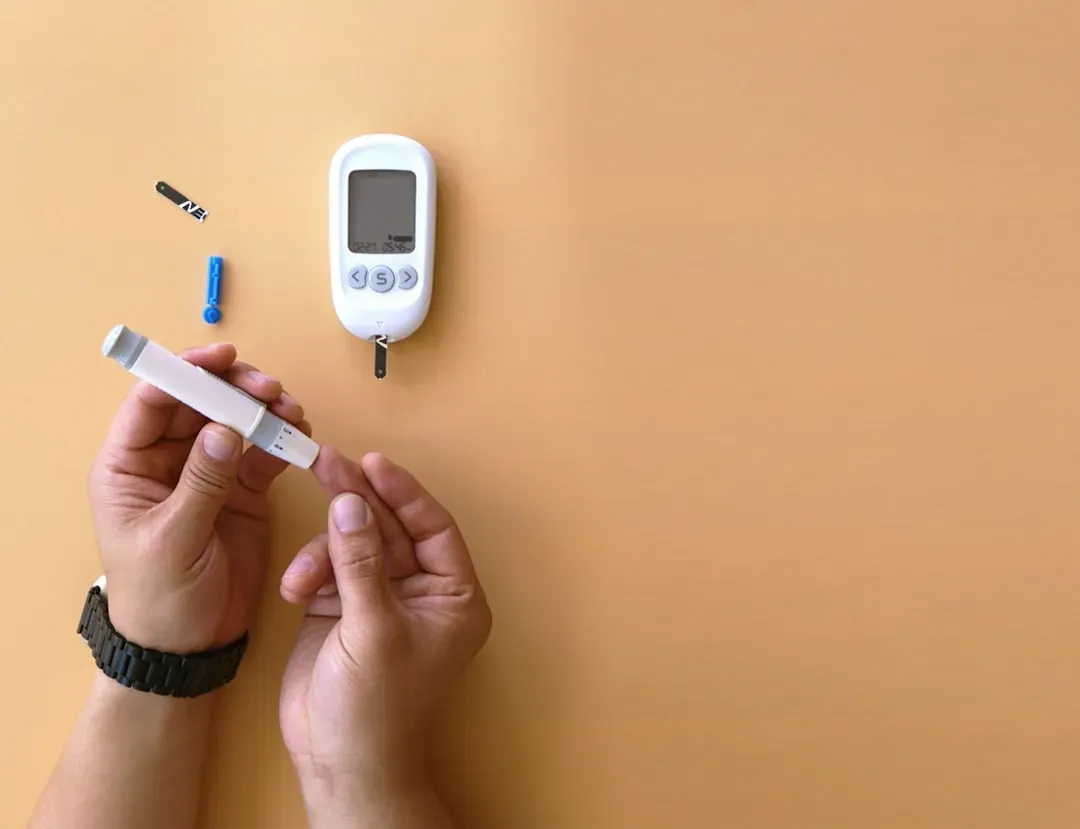
Most people check their blood sugar in the morning and call it done. But what you measure before bed is equally important – arguably more so when you’re trying to understand why your morning numbers keep creeping up. Consistent blood sugar monitoring helps you understand patterns that may indicate morning blood sugar spikes. You can use a home blood sugar monitor or a continuous glucose monitor to keep track of your readings. Along with a log of your food and activity, this can reveal hidden triggers.
The most effective way to diagnose or detect the dawn phenomenon as the cause of elevated morning blood sugar is with continuous glucose monitoring (CGM). CGM involves wearing a device that measures your glucose levels 24 hours a day – more specifically, every few minutes. The device uses this data to form a graph that shows a more complete picture of how your blood sugar levels change over time. That picture is invaluable. You might discover that you were actually trending high since midnight, not just after 3 a.m.
Even if you don’t have a CGM, a simple bedtime finger-stick reading written into a notebook each night builds a pattern over time. If the data shows you’re in range at bedtime, the culprit of morning highs is likely too little medication. You may go to bed with blood glucose levels within your target range, but that doesn’t mean they’ll stay that way overnight. Knowing which scenario applies to you is step one in actually fixing it.
Ritual 5: Review and Time Your Medications with Your Doctor

This last one requires a conversation, not just a habit change. But it may be the most clinically impactful ritual of all. If you take medication or insulin, ask your doctor about the best time to take it. They might suggest adjusting the dosage or timing of your evening medication or insulin to help avoid high blood sugar levels in the morning. It’s a deceptively simple intervention that makes a very real difference.
Changing the timing of your long-acting insulin injection, or switching to a twice-daily basal insulin or an ultra-long-acting insulin, might fix the problem. The dawn phenomenon affects roughly more than half of all people with either type 1 or type 2 diabetes, according to research published in StatPearls via the National Institutes of Health. The dawn phenomenon has been documented in both type 1 and type 2 diabetes and has been demonstrated in all age groups, even patients with type 2 diabetes over 70 years of age, with a prevalence estimated to exceed 50 percent for both types.
The evening replacement of basal insulin, which abolishes the dawn phenomenon by restraining hepatic glucose production and lipolysis, is an effective treatment as it mimics the physiology of glucose homeostasis in normal, nondiabetic subjects. This is not a one-size-fits-all answer, and it absolutely requires medical supervision. But bringing your bedtime glucose logs and CGM data to your next appointment gives your doctor the raw material to make a genuinely informed adjustment. That partnership is the whole game.
The Bottom Line

The dawn phenomenon is real, it’s common, and it’s not your fault. In the early hours of the morning, hormones including cortisol and growth hormone signal the liver to boost the production of glucose, which provides energy that helps you wake up. This triggers beta cells in the pancreas to release insulin to keep blood glucose levels in check. But if you have diabetes, you may not make enough insulin or may be too insulin resistant to counter the increase in blood glucose. Your body is just doing what bodies do – only without the backup system that most people take for granted.
The five rituals above aren’t magic. They’re small, consistent adjustments that work together over time, like tuning five different instruments until the whole orchestra plays in key. Some will make a bigger difference for you than others, and that’s fine. Start with one.
What would you try first – and has the dawn phenomenon ever caught you completely off guard? Share your experience in the comments.


