A Phenomenon With a Long History
The sensory hedonic phenomenon was first described in 1956 by the French physiologist Jacques Le Magnen. The term “sensory-specific satiety” was coined in 1981 by Barbara J. Rolls and Edmund T. Rolls. That formal naming opened the door to decades of systematic research into how the brain handles pleasure, appetite, and food variety.
Sensory-specific satiety is not just sensory and not simply habituation; it is a complex response to foods that includes not only immediate responses, but also a lifetime of learning about foods. In other words, your history with food matters just as much as what’s on your plate tonight.
What “Sensory-Specific Satiety” Actually Means

Sensory-specific satiety refers to the decrease in pleasantness of a food after repeated consumption, while other foods remain appealing. It’s a selective process. Your brain doesn’t just switch off appetite broadly; it tunes out the specific flavor and texture you’ve already been eating.
Sensory-specific satiety is driven by the sensory properties of food, for example taste, texture, colour, shape, and temperature. That means even something as subtle as changing from smooth to crunchy, or from savory to sweet, can reset a sense of interest in eating. The brain is essentially looking for novelty, not more calories.
The Brain Regions Behind the Effect
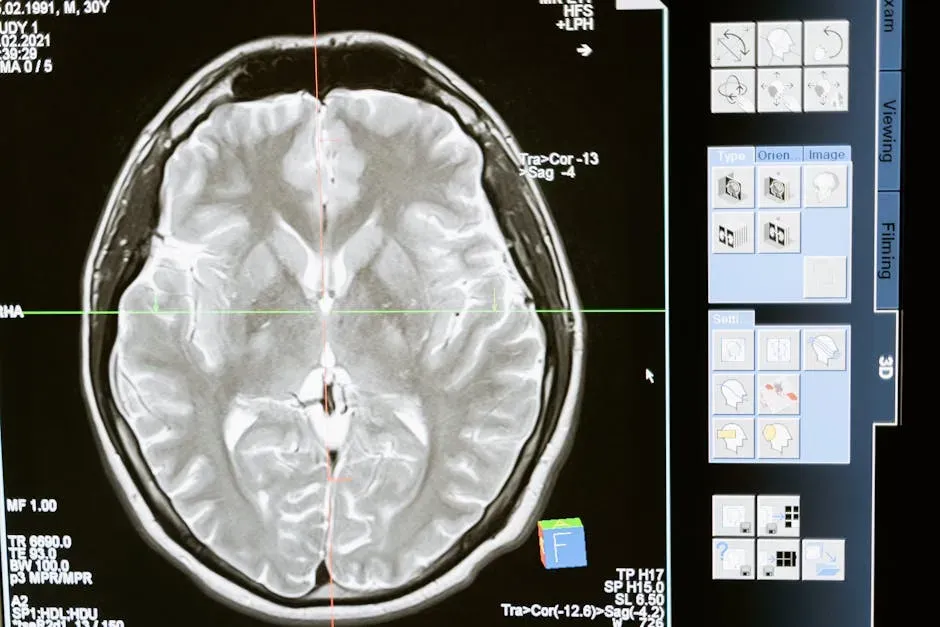
Research using brain imaging found that sensory-specific satiety was associated with a network of brain regions related to reward and taste processing, including the lateral orbitofrontal cortex. This region is closely tied to how pleasant we perceive a food to be, and its activity shifts noticeably as we continue eating the same thing.
Stimuli such as pleasant taste activate the orbitofrontal cortex. This activation declines when the same food is presented repeatedly, which is called sensory-specific satiety. The practical result is straightforward: the more you eat of something, the less exciting your brain finds it, until something new comes along.
The “Dessert Stomach” Is Real and It Lives in Your Brain

Researchers at the Max Planck Institute for Metabolism Research fed mice to the point of fullness and then gave them sugar. In doing so, they found that the same neurons signaling satiety, or fullness, also released β-Endorphin, a naturally-occurring opiate. This chemical bound to opiate receptors in the mice brains and triggered a feeling of reward.
The mice really went for the sugary feed, consuming six times more calories than when they had regular chow for dessert. That’s a striking number. When the sugar was replaced with more ordinary food, interest was minimal. The reward circuit was specifically activated by sweetness, not by additional calories alone.
The researchers found the same neural mechanism in humans when studying donated brain tissue and scanning the brains of volunteers, who sat in an fMRI machine and were fed a sugar solution through a tube. This led the scientists to conclude that in humans like in mice, “the opiate action in this part of the brain drives that consumption of high-sugar containing foods.”
Satiety Neurons That Flip Into Reward Mode
In the mice, researchers monitored the activity of neurons that are associated with feelings of fullness, called POMC neurons. They’re located in a part of the brain called the hypothalamus, which is “very important for promoting satiety,” according to Henning Fenselau, one of the study authors and a researcher at the Max Planck Institute for Metabolism Research in Cologne, Germany.
When mice are full and eat sugar, these nerve cells not only release signaling molecules that stimulate satiety, but also one of the body’s own opiates: β-endorphin. This acts on other nerve cells with opiate receptors and triggers a feeling of reward, causing the mice to eat sugar even beyond fullness. This opioid pathway in the brain was specifically activated when the mice ate additional sugar, but not when they ate normal or fatty food.
The Evolutionary Logic of Craving Sweets When Full

Interestingly, this mechanism was already activated when the mice perceived the sugar before eating it. In addition, the opiate was also released in the brains of mice that had never eaten sugar before. This suggests the response is deeply wired, not learned through experience or habit alone.
Henning Fenselau, one of the study authors, says this suggests that people’s brains evolved to love sugar in excess. “Because sugar is so easy to metabolize, its consumption beyond energy needs is favorable for animals,” he says. In environments where sweet foods were rare, consuming them whenever available made good evolutionary sense. Modern dessert culture, of course, is a very different situation.
The Role of Dopamine and Hedonic Hunger

Appetite is not governed solely by physical hunger. There is also “hedonic hunger,” the desire to eat because something is enjoyable or comforting. Sweet foods are particularly potent in this respect. They activate the brain’s mesolimbic dopamine system, heightening motivation to eat and temporarily weakening fullness signals.
When a person consumes a sugary dessert, they also get a hit of dopamine, a chemical in the brain associated with feelings of reward and pleasure. If eating dessert is a regular part of your daily routine, “the release of dopamine shifts from after you eat the food to the anticipation of eating the food.” This is what constitutes a craving, and it may make you more likely to reach for a slice of pie at the end of a big meal.
The Buffet Effect: When Variety Becomes Overconsumption

The more variety offered, the more people will eat. Thus, a larger amount of food will be eaten at a buffet because the variety of foods and flavors presented renews the desire to eat in the individual. This is sensory-specific satiety working in reverse, resetting appetite with each new dish.
In one study comparing a single-course meal with a four-course meal, participants consumed 60% more in the multiple-course condition. A separate classic study by Rolls and van Duijvenvoorde reinforced this: they fed participants four courses of the same food or four courses of different foods which included sausages, bread and butter, chocolate dessert, and bananas. The results revealed a 44% increase in overall food consumption when exposed to the meals with a variety of foods.
Sensory-specific satiety is likely adaptive since it drives consumption of a varied diet, which is useful to achieve a balanced diet. However, in the current obesogenic environment, the downside is that the availability of a wide variety of energy-dense foods can facilitate excess intake and potentially lead to obesity.
How Timing and Hormones Create a Window of Vulnerability

The gut-brain signalling that creates the sensation of fullness does not respond instantly. Hormones such as cholecystokinin, GLP-1, and peptide YY rise gradually and typically take between 20 and 40 minutes to produce a sustained sense of satiety. Many people make decisions about dessert before this hormonal shift has fully taken effect, giving the reward system space to influence behaviour.
Restaurants, consciously or otherwise, often time dessert offerings within this window. The arrival of the dessert menu just minutes after the main course is not random. It lands precisely when your hormonal fullness signals are still catching up with reality.
Can We Use This Science Practically?

Studies have shown that eating a limited variety of foods can result in monotony effects, which some have termed “long-term sensory-specific satiety.” By continuing to eat similar meals, a dieter can reduce their overall food intake and use sensory-specific satiety as a tool for weight loss. It’s a counterintuitive insight: less variety at meals may naturally reduce how much you eat.
Sensory-specific satiety varies depending on age, with older adults experiencing decreased sensory-specific satiety and adolescents experiencing enhanced effects. This age difference has practical implications for how different populations respond to food environments, from school cafeterias to care homes for older adults.
Ultimately, researchers hope this research can lead to a better understanding of sugar overconsumption, obesity, and more sophisticated weight-loss drugs. The 2025 findings from the Max Planck Institute in particular opened a new line of inquiry into how blocking opioid pathways might one day reduce compulsive sugar intake, potentially complementing existing treatments.
Conclusion: Your Brain Was Built for This

The fact that dessert always finds room isn’t really about willpower, or even hunger. It’s about a system designed over millions of years to keep animals eating varied, energy-rich foods whenever those foods were available. That system worked beautifully in a world of scarcity.
Today, understanding the science behind sensory-specific satiety at least gives us a clearer picture of what we’re actually up against. Knowing that the “dessert stomach” is a genuine brain mechanism, rooted in opioid reward circuits and ancient evolutionary drives, changes the conversation from one of discipline to one of biology.
The urge for something sweet at the end of a meal is not a failure. It’s your brain doing exactly what it was built to do. The more interesting question is what we choose to do with that knowledge.