The Second Brain You Never Knew You Had
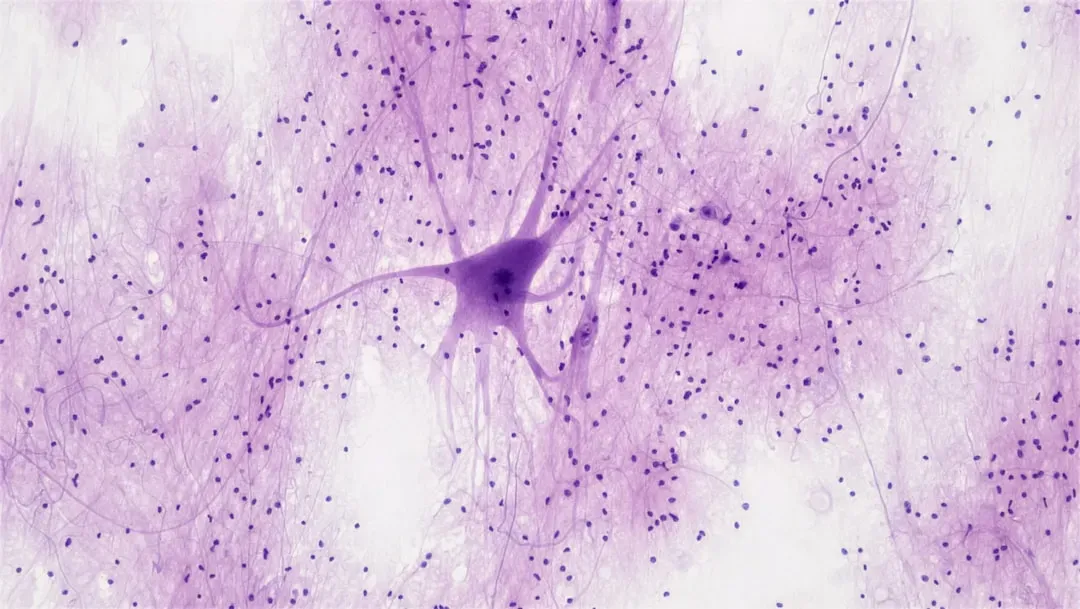
Hidden in the walls of the digestive system is what scientists call a “brain in your gut” that is revolutionizing medicine’s understanding of the links between digestion, mood, health, and even the way you think. Scientists call this the enteric nervous system, or ENS.
The ENS is two thin layers of more than 100 million nerve cells lining your gastrointestinal tract from esophagus to rectum. That’s a staggering number. To put it in perspective, that’s roughly the same number of neurons as found in a cat’s brain.
The ENS consists of a collection of neurons and glial cells that are responsible for peristalsis, secretion, and blood flow of the gastrointestinal tract. Its role goes far beyond digestion, though. Research now shows it actively participates in mood regulation and stress signaling.
The Gut-Brain Axis: A Two-Way Highway
One fascinating aspect of the gut’s widespread impact on health is its direct influence on and communication with the brain, a conduit known as the gut-brain axis. This is not a one-way street. Signals travel in both directions, continuously.
Research is increasingly recognizing that the genesis of anxiety involves not only neurochemical brain alterations but also changes in gut microbiota. The microbiota-gut-brain axis, serving as a bidirectional communication pathway between the gut microbiota and the central nervous system, is at the forefront of novel approaches to deciphering the complex pathophysiology of anxiety disorders.
The gut-brain axis plays a dominant role in maintaining homeostasis as well as contributing to mental health. The pathways that underpin it expand from macroscopic interactions with the nervous system to molecular signals that include microbial metabolites, tight junction protein expression, and cytokines released during inflammation. The dysfunctional gut-brain axis has been repeatedly linked to the occurrence of anxiety and depressive-like behaviors.
Your Gut Microbiome: The Invisible Orchestra
Much of the gut’s influence on the brain seems to be driven by the gut microbiome, the collection of usually beneficial bacteria and other microscopic organisms that reside in our digestive tracts. These microbes are far more than passive passengers in your intestines.
Bacteria in the gut microbiome play an intrinsic part in immune activation, intestinal permeability, enteric reflex, and entero-endocrine signaling. The gut microbiota communicates with the central nervous system through the production of bile acids, short-chain fatty acids, glutamate, GABA, dopamine, norepinephrine, serotonin, and histamine.
A bidirectional Mendelian randomization analysis by researcher Yaoyong Lai revealed that gut microbiota dysbiosis is a causative factor in depression and anxiety, rather than merely a consequence of these disorders. That distinction matters enormously for how we understand and treat these conditions.
The Serotonin Surprise
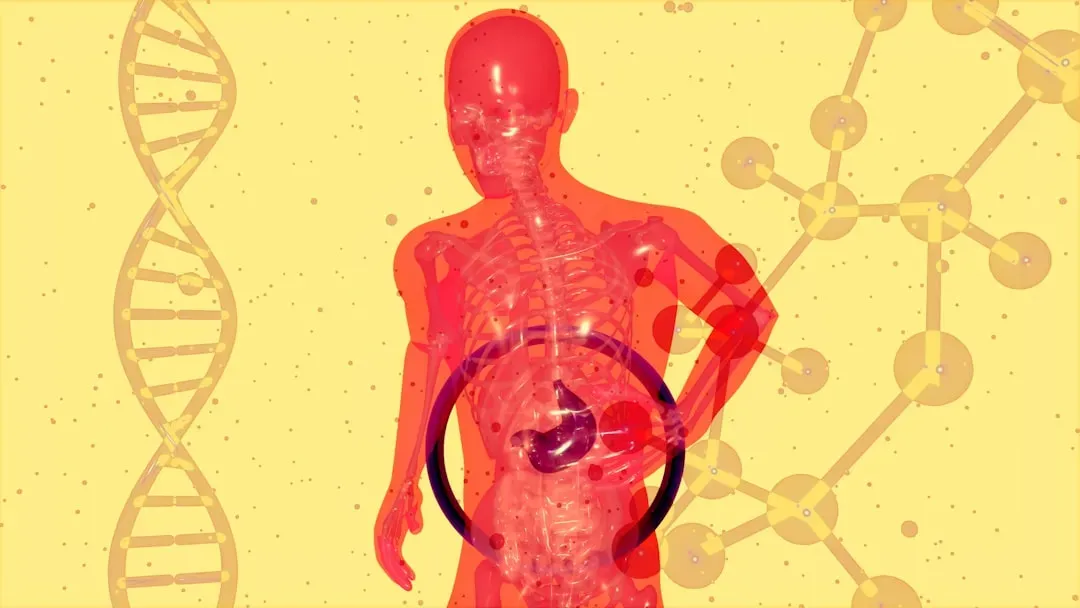
The assumption has long been that serotonin acts primarily within the brain. But this perspective neglects a remarkable biological fact: around 90 to 95 percent of the body’s serotonin is not in the brain at all. It’s produced in the gut.
Researchers have discovered new connections between the gut and brain that hold promise for more targeted treatments for depression and anxiety. A study published in the journal Gastroenterology shows that increasing serotonin in the gut epithelium, the thin layer of cells lining the small and large intestines, improves symptoms of anxiety and depression in animal studies.
The researchers also determined that vagus nerves, a key highway of communication between the digestive system and brain, are the path by which serotonin in the gut epithelium modulates mood. Cutting off this communication in one direction, from gut to brain, removed improvements in anxiety and depression.
The Vagus Nerve: Nature’s Mood Cable
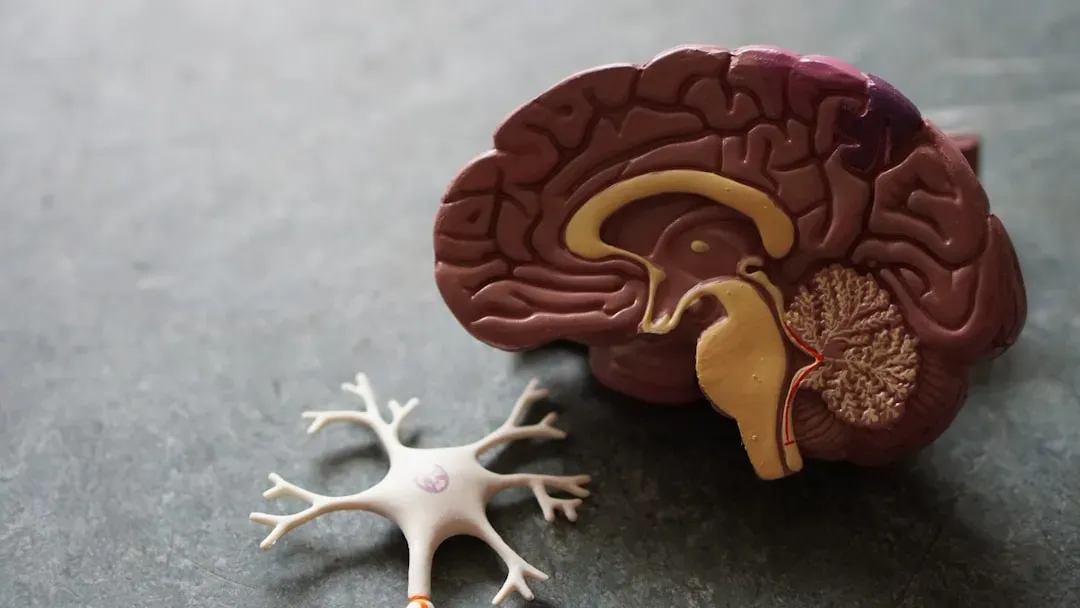
The vagus nerve is the most direct link out of all the potential paths in gut-brain communication, since various receptors on the vagal afferents sense and send signals from the gut to the brain. It has been discovered that the vagus nerve affects central nervous system reward neurons, which in turn affects mood and behavior.
Neuroactive compounds like gamma-aminobutyric acid, or GABA, synthesized by gut bacteria, impact stress response and anxiety through the vagal pathway. GABA is one of the main calming neurotransmitters in the brain, and its production starts, in part, in your intestines.
Certain bacterial genera have been shown to interact with the vagus nerve to decrease anxiety and depressive symptoms in both mice and humans. The increased presence of the Lactobacillus genus has been shown to decrease corticosterone levels and urinary-free cortisol levels, attenuate pro-inflammatory cytokines such as TNF-alpha and IL-6, and increase anti-inflammatory cytokines.
When the Gut Goes Wrong: Dysbiosis and Anxiety
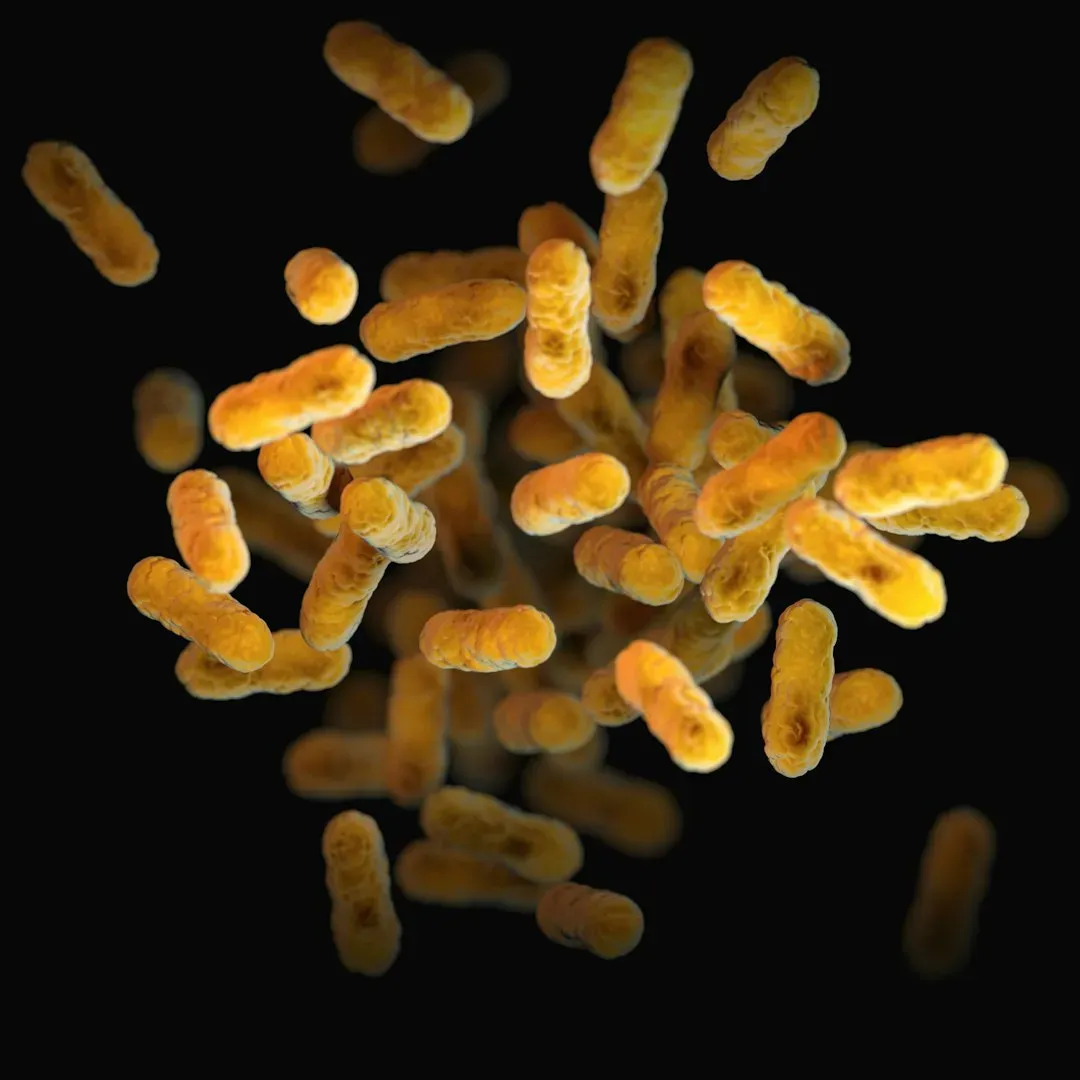
Recent research highlights the association between gut dysbiosis and psychiatric disorders including anxiety, depression, and stress-related conditions. Key findings indicate that altered microbial diversity, decreased short-chain fatty acid production, and increased neuroinflammation contribute to mental health disturbances.
Dysbiosis can lead to an overgrowth of harmful bacteria that produce lipopolysaccharides, or LPS, components of their outer membrane. LPS can trigger a strong immune response, and when they enter the bloodstream due to a “leaky gut,” they can contribute to systemic inflammation and potentially influence neuroinflammatory processes within the central nervous system.
Decreased gut microbial diversity may impair enteroendocrine cell activity and disrupt peptide secretion. Such disturbances could affect emotional states and behavior via gut-brain interactions, increasing vulnerability to anxiety and depression.
Stress Flows Both Ways
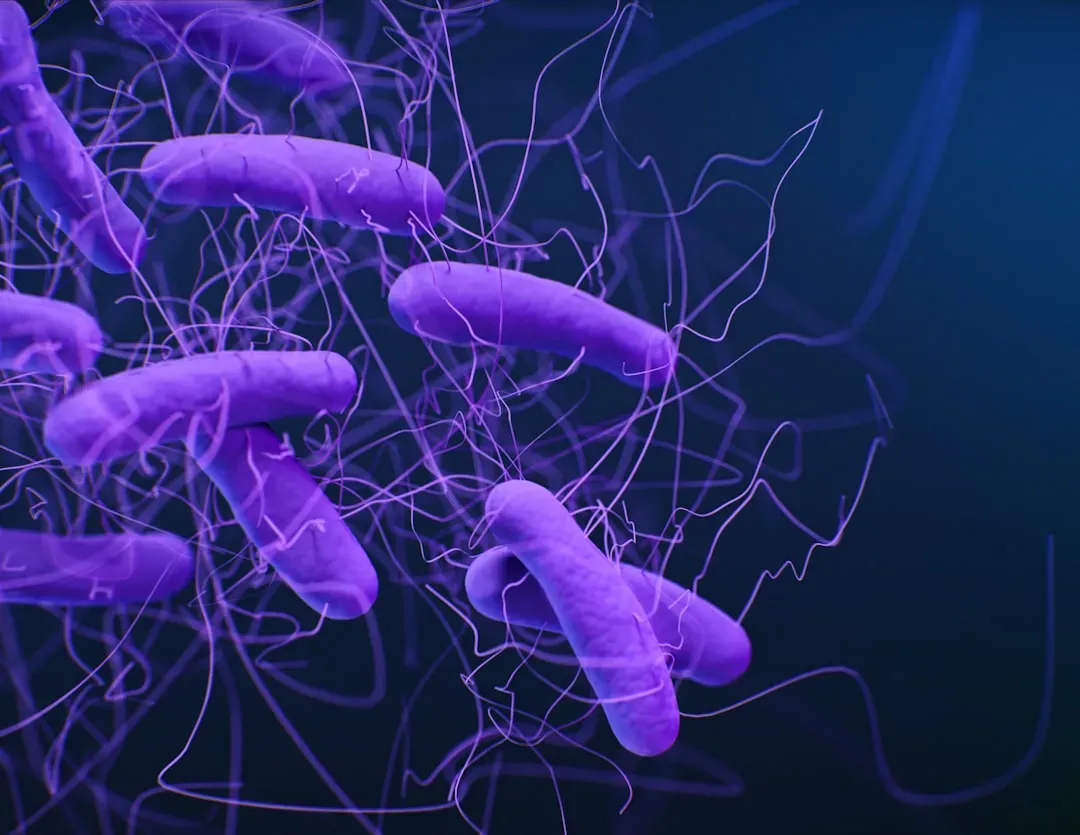
A person’s mental health can also impact their gut health. Psychological stress has been shown to impact the makeup of the gut microbiome, either indirectly through stressed people turning to comfort-food-heavy diets which in turn change their microbiome makeups, or directly through molecular signals that travel from the brain to the gut. Stress is often linked to pro-inflammatory bacterial species in the gut.
Exposure to psychosocial stress triggers the activation of the sympathetic nervous system and the hypothalamic-pituitary axis, leading to various physiological responses. However, chronic stress in susceptible individuals could cause sustained activation of these systems, leading to immune dysregulation consisting of redistribution of natural killer cells, decreased function of T and B cells, and elevation of pro-inflammatory cytokines.
Chronic stress disrupts the enteric nervous system activity, causing gut dysbiosis characterized by decreased levels of Bacteroides, Lactobacillus, and Bifidobacterium and increased intestinal permeability, further contributing to gastrointestinal disorders. In other words, an anxious brain creates an unhealthy gut, which in turn feeds more anxiety. It’s a cycle that can be difficult to break.
The Microbiome in Childhood: Anxiety Seeds Planted Early

The microbiome-gut-brain axis plays a critical role in mental health. Research linking the microbiome to brain function is limited particularly during development, when tremendous plasticity occurs and many mental health issues like depression and anxiety initially manifest.
Researchers have found that relative abundances of stress-sensitive gastrointestinal microbes at age two years predicts internalizing symptoms in middle childhood through altered emotion-related brain network connectivity. That’s a striking finding. The state of a toddler’s gut may shape how that child processes emotional stress years later.
Studies suggest that the composition of the gut microbiota is shaped from birth and continues to evolve in response to diet, the environment, and lifestyle. Early life disruptions to that ecosystem could have long-lasting effects on anxiety vulnerability well into adulthood.
Fecal Transplants, Probiotics, and the Future of Anxiety Treatment

Introducing gut bacteria into germ-free mice has been shown to reduce anxious behaviors in the animals, and fecal transplants from humans with depression into rats ramped up depression and anxiety-like behaviors. These experiments strongly suggest the microbiome itself is doing some of the emotional heavy lifting.
These insights open new avenues for understanding and treating anxiety and other mental disorders, suggesting novel treatment strategies that include manipulating gut microbiota. Techniques such as the use of probiotics, prebiotics, and fecal microbiota transplantation can modify the composition of gut microbiota and rebuild the gut environment, improving the psychological well-being of individuals.
Interventional approaches including probiotics, prebiotics, synbiotics, diet-based strategies, and fecal microbiota transplantation have shown modest benefits for depressive and anxiety symptoms, though findings remain mixed or preliminary in some areas. Promising, but the field is still young and requires much larger clinical trials before firm treatment protocols can be established.
What You Can Do Today: Diet, Lifestyle, and the Gut-Anxiety Loop

The Mediterranean diet has demonstrated effectiveness for anxiety and depression. This dietary pattern primarily includes olive oil as a fat source, abundant plant-based foods, fish, and limited intake of red meat, processed meat, and sweets. Such dietary patterns reduce oxidative stress and pro-inflammatory cell expression, both of which are key factors in depressive states.
Dietary influences on gut microbiota balance primarily involve the composition of microbial communities, gut permeability, inflammatory responses, and the metabolites produced by different microbial populations. For instance, diets rich in omega-3 fatty acids, such as those including fish oil, can enhance beneficial microbial communities, bolster gut barrier function, and decrease levels of circulating LPS, thus mitigating systemic inflammation.
Growing evidence suggests that targeted interventions aimed at restoring microbial balance, such as probiotics, prebiotics, and dietary modifications, may help with dysbiosis and offer promising therapeutic strategies for enhancing mental well-being and mitigating symptoms of neuropsychiatric disorders. These aren’t magic fixes, but they represent a genuine, evidence-backed starting point for anyone looking to take better care of both their gut and their mental health.
What the Research Still Doesn’t Know
Many studies support the role of the gut microbiome in the production of anxiety symptoms and suggest the potential for pro and prebiotics for their treatment, but there are also contradictory findings and concerns about the limitations of some research. Future research needs to consider longer-term studies incorporating factors such as sex of the subjects, drug use, comorbidity, ethnicity, environmental effects, diet, and exercise.
The long-term effects of interventions like fecal microbiota transplantation on the recipient’s microbiome and overall health are still unclear, making it crucial to develop standardized safety protocols. The lack of consensus on optimal treatment protocols, including the preparation, storage, and administration of fecal transplants, complicates its widespread clinical use. While FMT offers significant promise in restoring microbial balance, its effectiveness remains highly dependent on both the recipient’s microbiota composition and the specific microbial strains used.
Further research is needed to better understand the mechanisms through which gut microbiota influences brain function and to develop effective therapeutic interventions based on microbiome modulation. Future research should explore multi-strain probiotic combinations, personalized gut microbiota-targeted treatments, and the interaction between dietary modifications and microbiota composition in anxiety disorders.
Conclusion: A New Map for an Old Problem
Anxiety has been treated as a brain-only condition for the better part of a century. The science developing right now suggests that view was always incomplete. The gut is not simply a passive reactor to stress. It is an active participant, capable of generating the very signals that shape how anxious or calm you feel on any given day.
This doesn’t mean that every case of anxiety traces back to what you had for lunch, nor that a probiotic capsule will replace therapy or medication. The relationship is complex, bidirectional, and still being mapped in real time by researchers around the world.
What it does mean is that caring for your gut, through diet, reducing unnecessary antibiotic use, managing chronic stress, and staying curious about the science, is no longer just about digestion. It may be one of the most direct paths we have toward a calmer, more resilient mind. Sometimes the answers to what’s happening in your head start with what’s happening several feet below it.