For decades, fats have been painted as the villain in your diet. Low-fat products line supermarket shelves, and health authorities have long told us to cut back on anything remotely greasy. Yet despite all this fear mongering, our bodies desperately need these misunderstood nutrients. The truth behind dietary fats is far more nuanced than the simple good versus evil narrative we’ve been fed. Recent scientific evidence has started to flip the script on what we thought we knew about fats and cardiovascular health.
Let’s be real here: the fat debate isn’t settled just because new research emerges. Recommendations to limit dietary saturated fat intake are primarily drawn from observational studies rather than randomized controlled trials of cardiovascular disease prevention. Here’s the thing though: your brain, your hormones, and even your cells would quite literally fall apart without sufficient fat. It’s time to separate fact from fiction and explore exactly why your body craves what we’ve been conditioned to avoid.
Fats Build Your Brain and Keep It Sharp

Your brain isn’t just asking for fat, it’s practically made of it. The human brain is approximately 66 percent fat, and about 20 percent of that fat is omega-3. Think about that for a second: roughly two-thirds of the organ that controls everything you do consists of fatty tissue. Ingestion of omega-3 fatty acids increases learning, memory, cognitive well-being, and blood flow in the brain, according to a systematic review examining the effects on brain functions.
Higher omega-3 index was associated with larger hippocampal volumes, and consuming more omega-3s was associated with better abstract reasoning, findings from a study of over 2,000 participants revealed in 2022. The hippocampus plays a crucial role in learning and memory, so this isn’t a trivial detail. Perhaps most fascinating is research showing DHA and EPA, given in a combined supplement at prescription levels, improved cognitive function in older adults with coronary artery disease.
Even at midlife, the benefits are notable. Honestly, I find it striking that the worst outcomes occurred in people who had the lowest consumption of omega-3s, suggesting even modest intake can make a real difference.
Essential Vitamins Require Fat for Absorption

Ever wonder why some vitamins dissolve in water while others need fat? Vitamins A, D, E, and K are called the fat-soluble vitamins, because they are soluble in organic solvents and are absorbed and transported in a manner similar to that of fats. Without adequate dietary fat, your body simply cannot access these critical nutrients properly. The body absorbs fat-soluble vitamins into newly forming micelles in the small intestine, and this process relies on the secretion of bile and pancreatic enzymes.
Because fat-soluble vitamins are absorbed along with dietary fat, if a meal is very low in fat, the absorption of the fat-soluble vitamins in that meal may be impaired. You could be eating all the right vegetables and taking your supplements, but if you’re on an ultra-low-fat diet, you’re essentially flushing nutrients down the drain. Fat in food helps us absorb certain micronutrients, including vitamins A, D, K, and E, and we need a few grams of fat with each meal to absorb them effectively.
This explains why salad dressing isn’t just about taste. Research from 2025 showed that micellization increased the uptake of vitamin D3, vitamin E acetate, and vitamin K2 in human intestinal and buccal cell models, highlighting how fat delivery systems enhance vitamin bioavailability.
Hormones Depend on Fats as Building Blocks
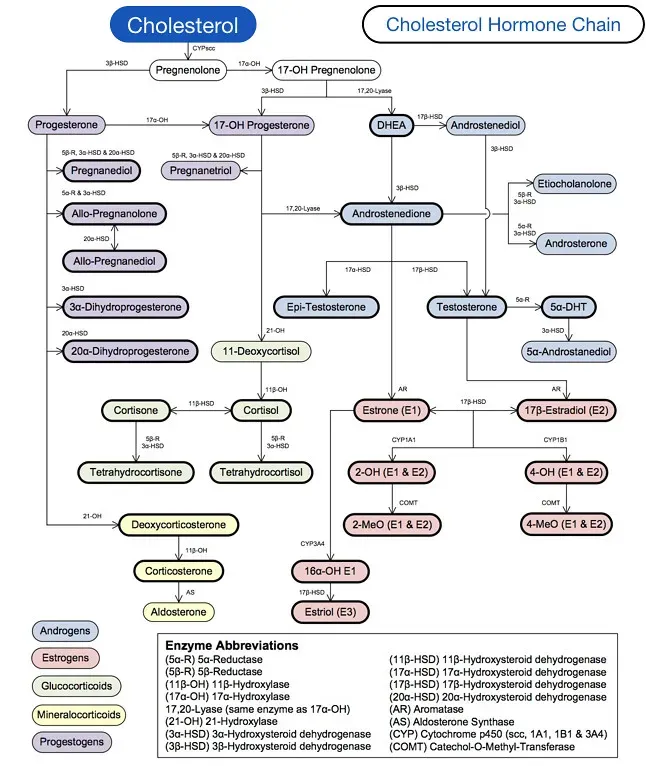
Here’s something that might surprise you: cholesterol is one of the key components of cell membranes and the precursor for testosterone, estrogen, and other essential hormones. Without adequate fat intake, your body struggles to manufacture the hormones that regulate everything from mood to metabolism to reproduction. Very low-fat diets can be detrimental to hormonal health, as healthy dietary fats are the essential building blocks for the production of key steroid hormones, including estrogen and testosterone.
Recent research found that the highest tertile of total fat intake was associated with increased total and free testosterone concentrations, with polyunsaturated fatty acids showing similar associations in women. The connection is clear across genders. A 2021 systematic review and meta-analysis discovered low-fat versus high-fat diets moderately decrease testosterone levels in men, via a reduction in testicular testosterone production.
Fat tissue can modify steroid hormones, converting one type into another, and produces nearly all of the estrogens in older women and up to half of the testosterone in reproductive-aged women. It’s complex and interconnected in ways nutritionists are still mapping out.
Cell Membranes Need Fat to Function
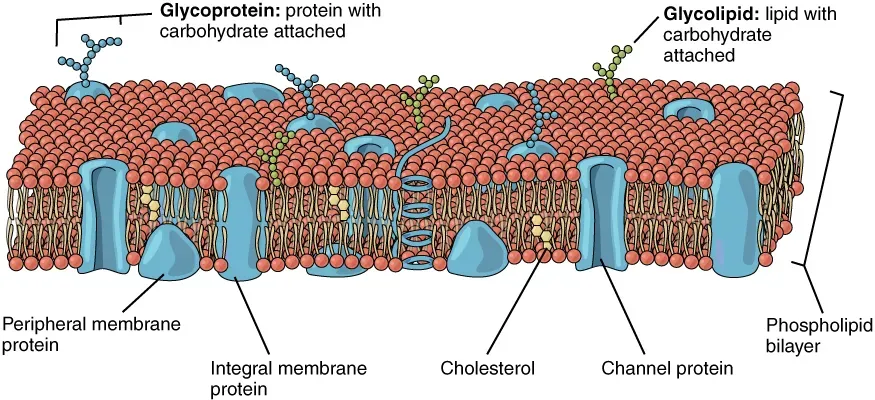
Every single cell in your body is wrapped in a membrane made primarily from fatty molecules. Without fats and related molecules your body would quite literally fall apart, because there would be no cell membranes to hold it together. Think of cell membranes as the gatekeepers that control what enters and exits each cell. Omega-3 fatty acids give membranes fluidity and elasticity, allowing brain cells to easily pass neurotransmitters, hormones, and proteins back and forth.
Lipids form membranes, are the basis of many chemical messengers and a major component of nerve cells, forming nearly 60 percent of the human brain. Without appropriate fatty acids in your diet, your cellular machinery starts operating like a rusty engine. Membrane integrity affects everything from nutrient absorption to waste removal to cellular signaling pathways. It’s truly foundational biology that highlights why fat isn’t optional – it’s essential.
The type of fats you consume directly impacts membrane composition and function. Your cells literally become what you eat, which makes the quality of dietary fats remarkably important.
Inflammation and Immune Function Are Regulated by Fats

Not all inflammation is bad, but chronic inflammation drives most modern diseases. Cells can turn omega-3 fatty acids into powerful anti-inflammatory molecules, allowing the brain to heal from trauma, infection, and oxidation or metabolic damage. This anti-inflammatory capacity extends throughout the entire body. DHA may exert neuroprotective effects through anti-inflammatory mechanisms, in part by competing with pro-inflammatory omega-6 fatty acids.
Omega-3 fats protect against pain and disorders like arthritis and joint problems, and in some studies, people with rheumatoid arthritis who took omega-3 supplements suffered less joint pain. The mechanism is fairly straightforward: omega-3 fatty acids compete with omega-6 fatty acids for the same metabolic pathways, and the end products from omega-3s tend to be less inflammatory.
The modern Western diet is skewed heavily toward omega-6 fatty acids from vegetable oils, creating an inflammatory imbalance. Restoring omega-3 intake helps rebalance this ratio and may quiet down the chronic inflammatory fires burning in many people’s bodies.
Some Fats May Actually Lower Heart Disease Risk

This is where things get controversial. Most recent meta-analyses of randomized trials and observational studies found no beneficial effects of reducing saturated fat intake on cardiovascular disease and total mortality, and instead found protective effects against stroke, according to a 2020 review published in the Journal of the American College of Cardiology. No significant differences in cardiovascular mortality, all-cause mortality, myocardial infarction, and coronary artery events were observed between intervention and control groups, and the findings indicate that a reduction in saturated fats cannot be recommended at present to prevent cardiovascular diseases and mortality, a Japanese systematic review concluded in 2025.
That doesn’t give you free rein to eat unlimited butter, though. A systematic review of 17 randomized clinical trials found that reducing intake of saturated fats reduced the chance of serious cardiovascular events, but only for some people. The nuance matters here: for patients at low cardiovascular risk, reducing saturated fat offers little or no benefit over a five-year horizon, but for those at high risk, there is an indication to replace saturated fat with polyunsaturated fat.
Substituting dairy with food sources of unsaturated fatty acids by adults and older adults may be associated with a lower risk of cardiovascular disease, based on evidence graded as limited. The key takeaway: it’s not simply about cutting fat but rather choosing the right types and considering your individual risk profile.
Energy Storage and Metabolic Flexibility Require Fat
Your body needs readily accessible energy reserves, and fat is the most efficient storage molecule available. While we’ve been taught to fear body fat, while obesity isn’t healthy, we need some fat tissue. Fat stores provide backup fuel when food isn’t immediately available and help regulate blood sugar by preventing dramatic spikes and crashes.
The balance of hormones and other signaling molecules can be disrupted without adequate fat tissue, and there are rare genetic conditions that prevent some people from storing fat, where patients often have insulin resistance and other metabolic problems similar to those seen in obesity. This paradox reveals that both extremes – too much and too little body fat – create metabolic dysfunction.
Additionally, one of fat’s most famous products is leptin, a signaling protein that suppresses appetite and increases energy use, and as fat tissue grows, it makes more leptin, suppressing hunger and halting weight gain, encouraging the body to maintain a stable weight. Fat tissue isn’t just passive storage; it’s an active endocrine organ communicating with your brain about energy status.
Fats Support Reproductive Health and Fertility

Extra fat is even more important for women, because their reproductive health depends on it. Women with extremely low body fat percentages often experience menstrual irregularities or amenorrhea because the body doesn’t have sufficient resources to support pregnancy. The polyunsaturated fatty acid docosapentaenoic acid was associated with increased progesterone and a reduced risk of anovulation, indicating that total fat intake is associated with very small increases in testosterone concentrations in healthy women and that increased docosapentaenoic acid was associated with a lower risk of anovulation.
Dietary fat intake could be linked to improved fertility, with intake of polyunsaturated fatty acids associated with very small increases in testosterone concentrations in healthy women and increased docosapentaenoic acid associated with a lower risk of anovulation, a 2016 study demonstrated. In other words, dietary fat intake could have a real impact on ovulation and therefore on one’s ability to get pregnant.
This isn’t just a female issue either. Adequate fat intake matters for male fertility too, since testosterone production – essential for sperm production – depends on sufficient dietary fat and cholesterol.
The Mediterranean Diet Shows Fat Can Be Healthy

Perhaps the strongest real-world evidence for healthy fat consumption comes from Mediterranean populations. The traditional Mediterranean diet has been widely recognized as a healthy model for eating, based on a massive body of evidence, yet it contains roughly forty percent of calories from fat, primarily olive oil, nuts, and fatty fish. Primary prevention of cardiovascular disease with a Mediterranean diet supplemented with extra-virgin olive oil or nuts has been demonstrated in clinical trials.
The Mediterranean diet, rich in fruits, vegetables, whole grains and healthy fats from sources such as olive oil and fish, is renowned for its anti-inflammatory properties and is associated with a lower risk of many chronic diseases, can help improve insulin sensitivity and support the production of adrenal and sex hormones. The diet works because it emphasizes quality fats rather than eliminating them entirely.
Healthy fats are plentiful in many whole foods, such as meats, poultry, eggs, omega-3 rich seafood, nuts, seeds, full-fat dairy, olives, and avocados, according to the newly released 2025-2030 Dietary Guidelines. This represents a notable shift toward recognizing that the source and quality of fats matter more than simply minimizing total fat intake.
The Type of Fat Matters More Than Total Fat Intake

Here’s where nutrition science has evolved considerably: the linear association between saturated fat intake and cardiovascular disease risk has been challenged, and it has been argued that simply reducing saturated fat intake without considering the replacement nutrients or the specific food sources is unlikely to yield significant health benefits. Different saturated fatty acids have different biologic effects, which are further modified by the food matrix and the carbohydrate content of the diet, and several foods relatively rich in saturated fats, such as whole-fat dairy, dark chocolate, and unprocessed meat, are not associated with increased cardiovascular disease or diabetes risk.
Saturated fat consumption should not exceed ten percent of total daily calories, and significantly limiting highly processed foods will help meet this goal, though more high-quality research is needed to determine which types of dietary fats best support long-term health. The focus has shifted from simply cutting fat to improving fat quality and reducing ultra-processed foods that often contain trans fats and damaged oils.
The science is clear: saturated fat consumption increases heart disease risk, saturated fat raises and polyunsaturated fat lowers LDL cholesterol, and lowering your LDL cholesterol cuts your risk of heart disease, according to the Center for Science in the Public Interest. Yet even this statement requires context about individual risk factors, replacement nutrients, and overall dietary patterns rather than isolated nutrient targets.
What have we learned from this deep dive into dietary fats? The black-and-white narrative we’ve been told for decades is crumbling under the weight of nuanced scientific evidence. Your body needs fats for countless functions, from building brain tissue to manufacturing hormones to absorbing vitamins. The real story isn’t about eliminating fats but choosing quality sources like fatty fish, nuts, avocados, and olive oil while minimizing ultra-processed foods. Did you expect the science to be this complex?




