The Global Sodium Problem We Still Haven’t Solved

The World Health Organization recommends that adults consume less than 5 grams of table salt per day, yet the global average intake is estimated at around 10.78 grams per day. That’s more than double the recommended limit for most of the world’s population. Closing that gap has proven stubbornly difficult.
Excessive sodium intake is considered a significant risk factor for cardiovascular disease, contributing to roughly 1.89 million CVD deaths in 2019. The WHO listed salt reduction as one of its five priority intervention strategies for non-communicable disease prevention and proposed a global target of a 30% reduction in sodium intake by 2025. Nevertheless, none of the WHO member states has reached that target.
Over the past three decades, the prevalence of hypertension in adults has doubled worldwide, surging from 650 million to 1.3 billion cases between 1990 and 2019. That trajectory tells us something important: relying solely on sodium reduction as a strategy is not working at scale. This is part of why potassium has drawn so much scientific attention.
What Potassium Actually Does in the Body

Potassium and sodium are closely interconnected but have opposite effects in the body. Both are essential nutrients that play key roles in maintaining physiological balance, and both have been linked to the risk of chronic diseases, especially cardiovascular disease.
High salt intake increases blood pressure, which can lead to heart disease, while high potassium intake can help relax blood vessels and excrete sodium while decreasing blood pressure. In practical terms, potassium works almost like a biological counterweight. When sodium tips the scale in one direction, potassium can help bring it back.
In addition to reducing salt intake, consuming sufficient amounts of vegetables and fruits rich in potassium is an essential non-pharmacological approach for hypertension management. Potassium not only lowers blood pressure but also prevents stroke and other cardiovascular diseases.
How Potassium Tells the Kidneys to Flush Sodium
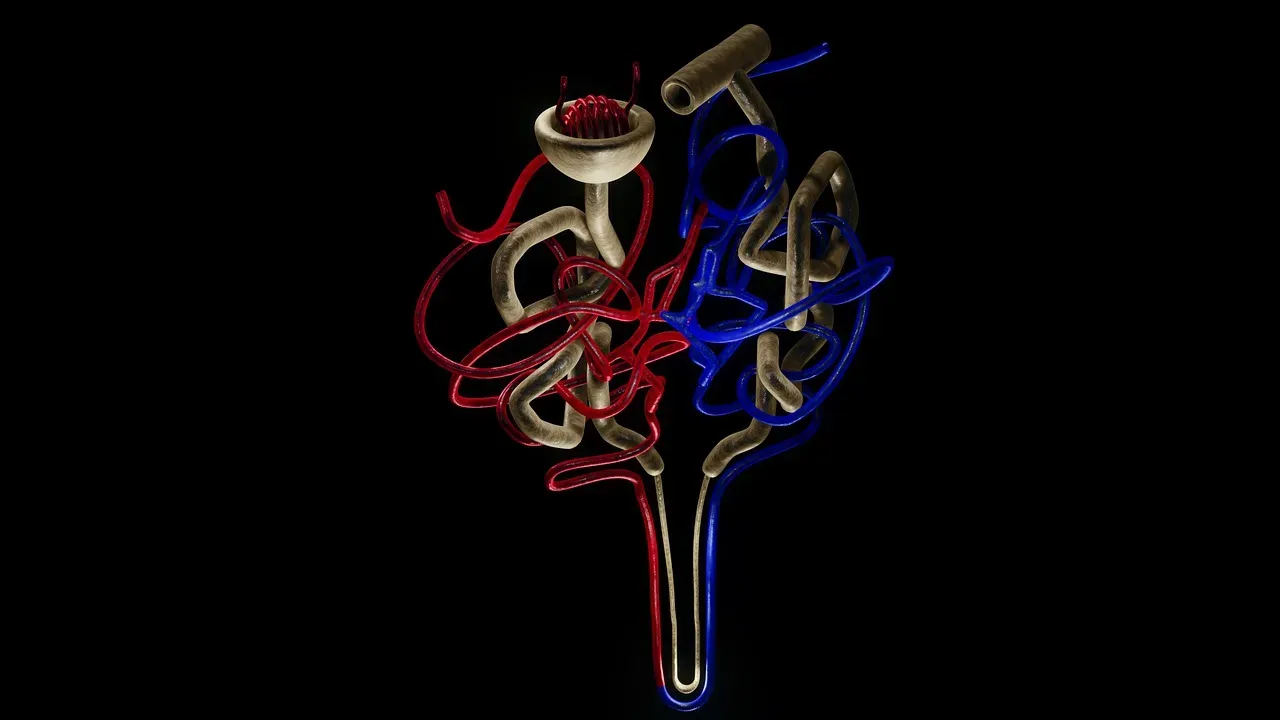
Recent studies have revealed that dietary potassium modulates the activity of the thiazide-sensitive sodium-chloride cotransporter in the distal convoluted tubule. The distal convoluted tubule acts as a potassium sensor to control the delivery of sodium to the collecting duct, the potassium-secreting portion of the kidney.
High potassium intake drives extracellular potassium concentration toward the top of its physiological range, exerting a thiazide-like effect on sodium excretion, thereby reducing extracellular fluid volume and blood pressure. This mechanism is remarkable because it means the body has a built-in pathway for using potassium to offload excess sodium through urine.
Multiple mechanisms are involved in the blood pressure-lowering and cardiovascular protective effects of potassium, one of which is natriuresis and the reduction in salt sensitivity. Potassium loading promotes aldosterone secretion, a well-known stimulator of renal salt reabsorption. Experimental studies have revealed that potassium loading suppresses renal salt reabsorption through mechanisms that do not require aldosterone. The kidney biology here is genuinely fascinating, and researchers are still mapping its full complexity.
The Sodium-to-Potassium Ratio: A More Telling Number

The sodium-to-potassium ratio appears to be more strongly associated with blood pressure than either sodium or potassium alone. This is one of the more important shifts in how nutritionists and cardiologists think about dietary risk. The ratio changes the frame entirely.
Dietary factors have increasingly been recognized as important contributors to cardiovascular health. Among them, the dietary sodium-to-potassium ratio has emerged as a promising indicator of dietary quality and cardiovascular risk.
The sodium-potassium ratio may be more important in actual situations than the individual effects of sodium or potassium. The WHO recommends a ratio of 1.0 based on molar units. Most people in high-income countries are eating far above that ratio, largely because processed food is loaded with sodium while being nearly devoid of potassium.
The Salt Substitute and Stroke Study: A Landmark Turning Point

In 2021, the Salt Substitute and Stroke Study (SSaSS), a prospective, open-label, cluster randomized controlled trial, involved 20,995 participants aged 60 years and older with hypertension across 600 villages in rural China. It tested the effect of table salt substitution with a potassium salt substitute containing 25% potassium chloride and 75% sodium chloride.
The observed systolic blood pressure reduction in SSaSS was minus 3.3 mmHg, with a corresponding mean reduction in 24-hour sodium excretion and a mean increase in 24-hour potassium excretion. Those numbers sound modest, but population-wide reductions in blood pressure of even a few millimeters of mercury translate into significant reductions in stroke and heart attack mortality.
In every model analyzed, the majority of the systolic blood pressure-lowering effect in SSaSS was estimated to be attributable to the increase in dietary potassium rather than the fall in dietary sodium. That finding reshaped the conversation considerably. It suggests potassium was doing the heavier lifting, not simply the reduction in salt.
New Research From 2025: Protecting Blood Vessels Too

Research presented at the American Physiological Society in April 2025 demonstrated that a high potassium intake attenuates the effect of a high-sodium diet on blood vessel function and reduces inflammatory markers. This extends the benefits beyond blood pressure readings into the actual health of vessel walls themselves.
The researchers concluded that their work, along with future research, may provide the impetus for revisiting current dietary guidelines for the American population to improve cardiovascular health and offset the harmful effects of a high-sodium diet. They next plan to study whether boosting potassium intake could be particularly beneficial in people at increased cardiovascular risk, such as those with high blood pressure and post-menopausal women.
That last point matters. Not all bodies respond equally to salt, and understanding which populations benefit most from potassium intervention is a critical next step for turning science into targeted clinical care.
Clinical Guidelines Are Catching Up

The Australian National Hypertension Taskforce Roadmap, published in 2024, recommends the inclusion of switching regular salt for potassium-enriched salt as a lifestyle therapy for blood pressure control. The recently updated 2024 European Society of Cardiology Guidelines for managing elevated blood pressure and hypertension now also include a specific recommendation for the use of potassium-enriched salt.
Specifically, in patients with hypertension without moderate-to-advanced chronic kidney disease and with high daily sodium intake, an increase of potassium intake by 0.5 to 1 gram per day, through sodium substitution with potassium-enriched salt comprising 75% sodium chloride and 25% potassium chloride, or through diets rich in fruits and vegetables, should be considered.
Consistent recent data from randomized controlled trials show that potassium-enriched, sodium-reduced salt substitutes are an effective option for improving consumption levels and reducing blood pressure and the rates of cardiovascular events and deaths. The evidence is no longer theoretical. It’s guideline-level strong.
Most People Are Not Getting Enough Potassium

The typical U.S. diet is imbalanced: Americans average about 3,300 milligrams of sodium per day, about three-quarters of which comes from processed foods, while only getting about 2,900 milligrams of potassium each day. That imbalance is the structural problem behind much of the hypertension epidemic.
Potassium is identified in the 2020 to 2025 Dietary Guidelines for Americans as a nutrient of concern because it is associated with health benefits but is under-consumed by most individuals. Meanwhile, the diets of many people in the United States provide less than recommended amounts of potassium. Even when food and dietary supplements are combined, total potassium intakes for most people remain below recommended amounts.
The estimated average daily intake of potassium in adults is about 2,320 milligrams for women and 3,016 milligrams for men. Compare that to the official Adequate Intake levels and the gap is clear for women in particular.
The Best Food Sources of Potassium

Many vegetables and fruits are rich sources of potassium. Many vegetables and fruits are rich sources of potassium. Milk and milk products also contain potassium. These food-based sources are considered preferable because they come with a full complement of fiber, vitamins, and phytonutrients that supplements simply cannot replicate.
Getting between 3,500 and 4,700 milligrams of potassium per day from tomatoes, spinach, sweet potatoes, and other fruits and vegetables may lower your risk of kidney stones, stroke, and high blood pressure. Those are foods most people already recognize as broadly healthy, which makes the dietary shift more practical than it might initially seem.
People with low intakes of potassium have an increased risk of developing high blood pressure, especially if their diet is also high in salt. Increasing the amount of potassium in your diet and decreasing the amount of sodium might help lower your blood pressure and reduce your risk of stroke. The two strategies reinforce each other, and neither cancels out the other.
Important Cautions: Who Should Be Careful

Salt substitutes containing potassium chloride should not be used by older people, people with diabetes, pregnant women, people with kidney disease, and people taking some antihypertensive drugs such as ACE inhibitors and angiotensin receptor blockers. This is a meaningful caveat that applies to a substantial portion of the population.
People who have chronic kidney disease and those who use certain medications can develop abnormally high levels of potassium in their blood, a condition called hyperkalemia. Examples of these medications include angiotensin-converting enzyme inhibitors and potassium-sparing diuretics. Hyperkalemia can occur in these people even when they consume typical amounts of potassium from food.
Before using potassium-based salt substitutes, it is important to check with a healthcare professional, especially if you have kidney disease or take medicines that affect potassium. For most healthy adults, increasing potassium from whole foods carries essentially no risk. The caution applies primarily to those with existing kidney impairment or on specific drug regimens.
The Bigger Picture: A Dual Strategy

There is an urgent need for policies that both reduce sodium and increase potassium intake. Identifying a strategy that fits cultural context will be key to improving population-wide blood pressures. No single dietary lever does everything, and the most compelling evidence now points toward working both sides of the equation simultaneously.
A simultaneous dietary intervention on sodium and potassium may be an easier approach to apply in the future, as tighter regulation of both intakes should have a greater impact on blood pressure control and, consequently, cardiovascular morbidity and mortality. The synergy between the two strategies is where the real public health opportunity lies.
Reducing sodium intake by limiting the use of regular salt during cooking and at the table, and by choosing low-salt foods, along with increasing potassium intake through higher consumption of fruits and vegetables, should remain core dietary recommendations for all patients with hypertension. That advice, grounded in years of clinical evidence, is now being echoed across major international health bodies.
The takeaway is straightforward: potassium is not a replacement for watching your sodium intake, but it’s a powerful ally that most people are significantly underusing. Eating more vegetables, fruits, and whole foods isn’t a new idea, but understanding exactly why it protects the heart adds a layer of precision to dietary choices that can make a real difference over time.



